Case Report, J Biochem Physiol Vol: 7 Issue: 4
Reverse Takotsubo and Prolonged Cardiac Arrest Following Inadvertent Epinephrine Injection
Adrien Gross1*, Sebastien Colombier2, Magali Neves3 and Christian Balmer1
1Department of Anesthesia, Valais Hospital, Av. du Grand-Champsec 80, 1951 Sion, Switzerland
2Department of Cardiac Surgery, Valais Hospital, Av. du Grand-Champsec 80, 1951 Sion, Switzerland
3Department of Intensive Care, Valais Hospital, Av. du Grand-Champsec 80, 1951 Sion, Switzerland
*Corresponding Author: Adrien Gross,
Department of Anesthesia, Valais
Hospital, Av. du Grand-Champsec 80, 1951 Sion, Switzerland
E-mail: adrien.gross@hopitalvs.ch
Received date: 26 September, 2024, Manuscript No. JBPY-24-148904;
Editor assigned date: 30 September, 2024, PreQC No. JBPY-24-148904 (PQ);
Reviewed date: 14 October, 2024, QC No. JBPY-24-148904;
Revised date: 22 October, 2024, Manuscript No. JBPY-24-148904 (R);
Published date: 30 October, 2024, DOI: 10.4172/jbpy.1000174.
Citation: Gross A, Colombier S, Neves M, Balmer C. (2024) Reverse Takotsubo and Prolonged Cardiac Arrest Following Inadvertent Epinephrine Injection. J Biochem Physiol 7:4.
Abstract
Reverse and classical forms of Takotsubo cardiomyopathy are typically seen in situations with high levels of catecholamines or by catecholamine administration such as epinephrine. We describe the case of a 27-year-old male who developed Reverse Takotsubo and cardiac arrest after inadvertent epinephrine administration during general anesthesia for minor orthopedic procedure. The patient underwent prolonged CPR and fully recovered normal left ventricular function and did not suffer any neurological sequelae. Anaesthesia safety and medication errors are discussed, as well as factors contributing to errors. Lessons should be learned from errors, and strategies to improve safety in anesthesia practice must be developed.
Keywords: Takotsubo cardiomyopathy; Epinephrine; Resuscitation; Medication error; Anesthesia safety
Introduction
Takotsubo Cardiomyopathy (TTC) is an acute and transient cardiac disease that resembles Acute Coronary Syndrome (ACS) in the absence of a coronary lesion [1]. The usual pattern is characterized by akinesia of apical and midventricular segments and hyperkinesia of basal segments [2,3]. However, in rare cases, TTC can present in a reverse fashion with basal and mid ventricular akinesia and apical hyperkinesia [4]. Triggers for TTC typically include stressful event or major emotional event where high levels of circulating catecholamines are found [5]. General anesthesia requires multiple drug administrations under continuous surveillance. On certain occasions, drugs must be prepared and administrated urgently, sometimes without double check, making these situations more prone to errors.
Case presentation
We present the case of a 27-year-old man (185 cm, 75 kg) without treatment or medical history. After a motorcycle accident, the patient was suffering from rupture of the biceps tendon and was scheduled for biceps tenodesis under general anesthesia..
A pre-operative analgesic interscalene block was performed with 30 ml of ropivacaïne 0.25% without any complications and in particular without any sign of local anaesthetic toxicity. Induction of anesthesia was well tolerated using propofol, sufentanil and rocuronium. Antibioprophylaxis with cefuroxime was administered 30 minutes prior skin incision without any adverse reactions.
In our institution, anesthetic drugs and syringes are prepared daily by anesthetist nurses. In this case, the anesthetist nurse filled a 10 ml syringe with epinephrine at a concentration of 1 mg/ml instead of phenylephrine at 0.1 mg/ml, subsequently labeling it with a standard phenylephrine tag. After 40 minutes of surgery, the patient exhibited progressive hypotension (with a minimal systolic pressure of approximately 70 mmHg). This hypotension was treated with 1 ml of the phenylephrine-labeled syringe containing epinephrine and the patient received 1 mg of epinephrine instead of 0.1 mg.
Immediately after injection, the patient developed sinus tachycardia of up to 180 bpm and hypertension, with a systolic of more than 220 mmHg. After two minutes, his rhythm progressed to Ventricular Fibrillation (VF). Cardiopulmonary Resuscitation (CPR) was immediately initiated and, according to American Heart Association (AHA) guidelines for cardiopulmonary resuscitation, the patient received 1 mg of epinephrine, 300 mg of amiodarone and two shocks of 200 J each [6]. After 5 minutes of CPR, the patient returned to sinus rhythm. Shortly after, due to persistent hypotension, the patient received another milliliter of the syringe supposed to contain phenylephrine. Immediately after, the patient developed again tachycardia and hypertension, followed by a second cardiac arrest secondary to VF. At this time, given the abnormal and excessive reaction to phenylephrine after the two uses, the syringe was suspected of containing something other than phenylephrine and was placed aside.
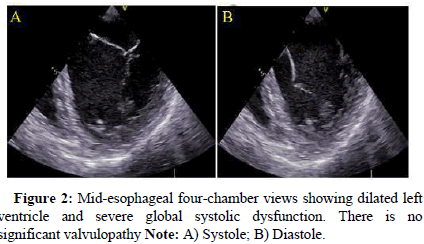
The patient received again 1 mg of epinephrine, 150 mg of amiodarone and two shocks. After the second shock, the rhythm degenerated into Pulseless Electrical Activity (PEA). Ongoing manual chest compressions were replaced by automated mechanical CPR using LUCAS Chest Compression Machine (CCM) 3, (Stryker, Michigan USA). A focused echo excluded a pneumothorax or an aortic dissection and revealed severe global hypokinesia with an estimated LVEF below 20%. At this time, local anesthetic intoxication was considered but the probability was judged low given the absence of symptoms at the time of the ropivacaïne injection and the long delay between the performance of the peripheral block and the cardiac arrest. A central femoral line was inserted and norepinephrine 10 μg/min and epinephrine 10 μg/min infusions were initiated before the transfer of the patient under mechanical CPR to a secondary hospital with cardiac surgery and Extracorporeal Membrane Oxygenation (ECMO) facilities. On arrival at the hospital after 70 minutes of CPR, the patient recovered a stable sinus rhythm under infusion of epinephrine and norepinephrine. A transoesophageal echocardiography performed on arrival showed a dilated left ventricle with severe dysfunction (Figures 1 and 2).
The patient was admitted in ICU where ECG remains unparticular. A transthoracic echocardiography repeated 4 hours after admission showed an image of Reverse Takotsubo with akinetic basis and preserved apical contraction (Figure 3).
After cessation of sedation, the patient recovered without neurologic complications. Under supportive care, he could be removed from inotrope support and extubated 8 hours after his ICU admission. His cardiac rhythm remains uneventful throughout his entire stay in ICU and cardiac intermediate care. He only complained of moderate chest pain secondary to mechanical CPR, adequately controlled with oral acetaminophen and oxycodone. The patient underwent a full cardiologic examination with coronary angiography and cardiac MRI. No structural abnormality or lesion was found. Echocardiography performed one month later revealed complete left ventricular recovery with normal LVEF (63%) without major abnormal wall motion except for only minor mid-inferior segmental hypokinesis. The patient had no chest pain and/or shortness of breath (Figure 4).
The syringe used during the anesthesia was sent for analysis to a university forensic lab, where the presence of epinephrine (1 mg/ml) was confirmed.
Discussion
Catecholamine-induced Takotsubo and Reverse Takotsubo have been previously described following epinephrine injection [7,8]. Reverse Takotsubo, a variant of the classical TTC, is more frequently seen in a younger population and patients normally fully recover LVEF within days or hours. In our case, the reaction to catecholamines was extremely severe and caused refractory cardiac arrest requiring prolonged CPR. The patient was even considered for ECMO before he spontaneously recovered.
This case shows that catecholamine susceptibility is extremely variable among population with reactions ranging from mild hypertension to refractory cardiac arrest. However, immediate initiation and efficient CPR allows full recovery without neurologic complications, even after prolonged CPR duration.
This case also highlights the importance of medication safety in the operative room and the potential patient harm of medications errors, which in some cases might even be fatal. As already widely published, medications errors are relatively frequent in anaesthesia practice with a rate of approximately 1 in 20 perioperative medication administrations that results in a medication error and/or an adverse drug event [9,10]. More than one third of these errors led to observed patient harm and the remaining two thirds had the potential for patient harm. Medication safety during anesthesia care is a complex problem with potential numerous harmful consequences due to the wide population exposed to anaesthesia worldwide [11]. The perioperative drug administration today often bypasses standard safety checks and in some situations these drugs need to be prepared and administrated urgently to treat life-threatening complications. Potential strategies to improve drug ampoule and packaging design are needed and are currently being investigated.
Another important point is the implementation of strategies and barriers to improve safety and minimize potential errors during anesthesia practice. Implementing human factors strategies in anesthesia has the potential to reduce the reliance on exceptional personal and team performance to provide safe and high-quality patient care. To encourage the adoption of human factors science in anaesthesia, the difficult airway society and the association of anaesthetists established a list of 12 recommendations [12]. These recommendations are categorized into four domains: Design (of environment, equipment and systems), barriers (which trap errors), reduction (which reduce the consequences of errors) and education and training. In situation, 10 ml ampoules of epinephrine were immediately removed from our anesthesia practice and a dedicated resuscitation cart was created. Also of importance is the debriefing and psychological support for all the staff involved in the critical event [13]. The death, or potential serious harm to a patient in an operating theatre may have a devastating effect on staff involved; the so-called second victim [14]. This second victim syndrome is equivalent to posttraumatic stress disorder and has both personal and professional consequences and should therefore always be recognized and sometimes treated. To improve patient safety, it is also vital to learn from cases that go well as from cases that do not.
Conclusion
Medication administration in the perioperative setting and patient safety is a major concern, due to the large number of different drugs and the multiple manipulations needed in anaesthesia and the wide population exposed to these potentially serious errors. When such errors occur, the patient must always be informed and the whole staff should debrief as psychological support might be needed.
References
- Y-Hassan S, Tornvall P (2018) Epidemiology, pathogenesis, and management of takotsubo syndrome. Clin Auton Res 28:53-65.
[Crossref] [Google Scholar] [PubMed]
- Ghadri JR, Wittstein IS, Prasad A, Sharkey S, Dote K, et al (2018) International expert consensus document on Takotsubo syndrome (part I): Clinical characteristics, diagnostic criteria, and pathophysiology. Eur Heart J 39(22):2032-2046.
[Crossref] [Google Scholar] [PubMed]
- Scantlebury DC, Prasad A (2014) Diagnosis of takotsubo cardiomyopathy. Circ J 78(9):2129-2139.
[Crossref] [Google Scholar] [PubMed]
- Templin C, Ghadri JR, Diekmann J, Napp LC, Bataiosu DR, et al. (2015) Clinical features and outcomes of takotsubo (stress) cardiomyopathy. N Engl J Med 373(10):929-938.
[Crossref] [Google Scholar] [PubMed]
- Wittstein IS, Thiemann DR, Lima JA, Baughman KL, Schulman SP, et al. (2005) Neurohumoral features of myocardial stunning due to sudden emotional stress. N Engl J Med 352(6):539-548.
[Crossref] [Google Scholar] [PubMed]
- Perman SM, Elmer J, Maciel CB, Uzendu A, May T, et al. (2024) 2023 American Heart Association Focused Update on Adult Advanced Cardiovascular Life Support: An Update to the American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation (5):254-273.
[Crossref] [Google Scholar] [PubMed]
- Nassif J, Nahouli H, Khalil A, Mikhael E, Gharzeddine W, et al. (2017) Epinephrine-induced Takotsubo cardiomyopathy during laparoscopic myomectomy: Case report and review of the literature. J Minim Invasive Gynecol 24(6):1037-1039.
[Crossref] [Google Scholar] [PubMed]
- Khoueiry G, Abi Rafeh N, Azab B, Markman E, Waked A, et al. (2013) Reverse Takotsubo cardiomyopathy in the setting of anaphylaxis treated with high-dose intravenous epinephrine. J Emerg Med 44(1):96-99.
[Crossref] [Google Scholar] [PubMed]
- Grigg EB, Martin LD, Ross FJ, Roesler A, Rampersad SE, et al. (2017) Assessing the impact of the anesthesia medication template on medication errors during anesthesia: A prospective study. Anesth Analg 124(5):1617-1625.
[Crossref] [Google Scholar] [PubMed]
- Nanji KC, Patel A, Shaikh S, Seger DL, Bates DW (2016) Evaluation of perioperative medication errors and adverse drug events. Anesthesiology 124(1):25-34.
[Crossref] [Google Scholar] [PubMed]
- Cranshaw J, Gupta KJ, Cook TM (2009) Litigation related to drug errors in anaesthesia: An analysis of claims against the NHS in England 1995–2007. Anaesthesia 64(12):1317-1323.
[Crossref] [Google Scholar] [PubMed]
- Kelly FE, Frerk C, Bailey CR, Cook TM, Ferguson K, et al. (2023) Implementing human factors in anaesthesia: guidance for clinicians, departments and hospitals: Guidelines from the Difficult Airway Society and the Association of Anaesthetists. Anaesthesia 78(4):458-478.
[Crossref] [Google Scholar] [PubMed]
- Brooks SK, Rubin GJ, Greenberg N (2019) Traumatic stress within disaster-exposed occupations: Overview of the literature and suggestions for the management of traumatic stress in the workplace. Br Med Bull 129(1):25-34.
[Crossref] [Google Scholar] [PubMed]
- Ozeke O, Ozeke V, Coskun O, Budakoglu II (2019) Second victims in health care: Current perspectives. Adv Med Educ Pract 12:593-603.
[Crossref] [Google Scholar] [PubMed]
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi