Case Report, Endocrinol Diabetes Res Vol: 9 Issue: 1
A Pituitary Macroadenoma Apoplexy
Yahya W Shihadeh*
Department of Endocrinology, Mouwasat Hospital, Khobar, Saudi Arabia
*Corresponding Author: Yahya W Shihadeh
Department of Endocrinology, Mouwasat Hospital, Khobar, Saudi Arabia,
Tel: + 966560595607;
E-mail: yashihi@yahoo.com
Received date: 20 January 2023, Manuscript No. ECDR-22-64548;
Editor assigned date: 24 January 2023, PreQC No. ECDR-22-64548 (PQ);
Reviewed date: 07 February 2023, QC No. ECDR-22-64548;
Revised date: 20 February 2023, Manuscript No. ECDR-22-64548 (R);
Published date: 27 February 2023, DOI: 10.4172/2470-7570.1000015.
Citation: Shihadeh YW, (2022) A Pituitary Macroadenoma Apoplexy. Endocrinol Diabetes Res 9:1.
Abstract
A case of acute pituitary apoplexy. The non-surgical conservative management successfully relieved symptoms. The main message here is that acute headaches in preexisting pituitary adenoma should be taken seriously and the early and accurate management of apoplexy can avoid many complications.
Keywords: Cabergoline; Paracetamol; vitamin B12; Ondansetron; Macroadenoma
Introduction
A 31 years old woman with a past medical history of pituitary adenoma, using Cabergoline (DOSTINEX) 0.5 mg tablet twice per week for 2 years, which could control the elevated levels of serum prolactin.
For a severe and new-onset headache (2 days), she initially applied to a primary clinic where medications for migraine (Eletriptan 40 mg tablet once as needed, paracetamol, and vitamin B12 tablet) were prescribed. However, her symptoms of headache, nausea/vomiting, changes in visual clarity, malaise, and weakness increased progressively. On the next day, she applied to our endocrinology clinic. At the examination, vital signs were unremarkable except for mildly low blood pressure 100/65 mmHg (other vitals: pulse 80/ minute, Temperature 36.8°C, respiratory rate 18/minutes), headache scale 8/10, dizzy feelings, no neurologic or visual field deficits.
The initial lab tests were unremarkable (basal cortisol 252 nmol/L, TSH 2.3 (0.4-4.2), FT4 13 pmol/L (10-28 pmol/L), prolactin 111 mIU/L (70-395 mIU/L). Other tests (serum electrolytes, CBC, ESR, LDH, creatinine, and GGT) were normal. The urgent MRI of the pituitary gland with contrast showed “a well-defined macroadenoma 13 x 12 x 11 mm a long maximum TS, CC and AP dimensions,respectively. The adenoma is 2 mm just beneath the optic chiasm. There was a view of hyperintensity on T1 and a relatively low signal on T2 suggestive of acute hemorrhage.”
Case Presentation
The diagnosis of acute pituitary macroadenoma apoplexy was established both clinically and radiologically. Immediately, the patient was treated as an out-patient for 2 reasons: Firstly, the team approach with ophthalmology and neurosurgery determined that the surgical intervention was not indicated. Secondly, upon the decision of a non-surgical management, insurance company rejected the coverage for the patient’s admission. Therefore, the patient was treated with these oral medications: prednisolone 20 mg tablet/day for 5 days, cabergoline 0.5 mg tablet twice per week, ondansetron 8 mg tablet BID, and ranitidine 300 mg tablet OD (metoclopramide and PPI were avoided due to their potential effects in rising prolactin) [1]. The patient was advised to get rest, avoidance of stress, have good sleep, and stay in a comfortable area [2]. She showed improvement in symptoms after 5 days of the treatment, and her symptoms resolved completely after one week [3]. The necessary laboratory tests which were done 3 weeks after the event showed unremarkable results (including the ACTH stimulating test (250 ug ACTH and testing serum cortisol at 0, 30, and 60 minutes) (Figure 1).
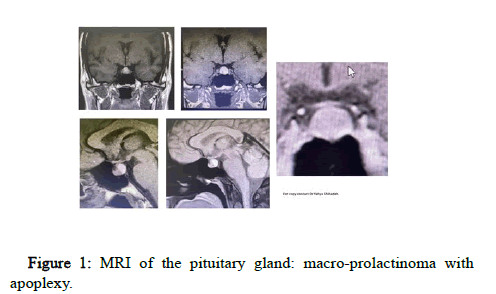
Figure 1: MRI of the pituitary gland: macro-prolactinoma with apoplexy.
Results and Discussion
This is a typical presentation of a mild case of acute apoplexy of a pituitary adenoma. Apoplexy of the pituitary gland is defined as bleeding inside a pre-existing adenoma, mainly due to its vascular compressive effects. Apoplexy occurs in about 10% of all adenomas [4]. Interestingly, it happens more frequently in male cases [5]. If we compare the features of this case with the most commonly reported symptoms in related literature, it seems that this patient has mild symptoms without complications [6].
The possible neuro-ophthalmologic complications and their underlying pathogenesis were summarized in the Table 1.
Table 1: The reported symptoms and their pathogenesis.
There were different factors reported in PUBMED literature that can cause bleeding inside about 10% of the pituitary adenomas. These risk factors were shown in Figure 2.

Figure 2: Risk factors for pituitary apoplexy.
In our reported case, the underlying causes could be the prolonged usage of cabergoline, though it was not definitive. An explanation: Shrinkage and subsequently hemorrhagic attack might occur inside the adenoma [7]. In reality, we looked back at the initial size of this patient’s MRI report 2 years ago, the adenoma size was 2 mm larger in all dimensions.
The mild hypotension of our patient (100/70 mmHg) whether it was a usual patient’s pressure, a trigger, or a sequence was not clear.
The medical treatment includes corticosteroids (Example. prednisolone or hydrocortisone over a few days), rehydrations, analgesics, and antiemetics. The indications for decompressive surgery are limited to the following situations: deterioration of visual acuity or fields, hemiparesis, and altered conscious level. Actually, the majority of apoplexy cases were managed medically with careful observations [8]. The prognosis clearly depends on the presence of acute or later complications. Therefore, a long-term follow-up is crucial. It includes repeated assessments of the pituitary and visual functions after 4-6 weeks of the event. In this case, a repeated assessment showed no new abnormal findings. It is important to mention that the recurrence rate of apoplexies was reported up to 11% in the subsequent 6 years [9].
Conclusion
We reported a case of pituitary apoplexy with complete resolution of symptoms after a week by proper conservative management as an outpatient. The main message to be conveyed is that an early and accurate diagnosis of apoplexy prevents many complications of this life-threatening condition.
References
- Lissoni P, Cazzaniga M, Rovelli F, Mainini E, Tancini G, et al. (1994) Ondansetron does not stimulate prolactin release in breast cancer patients. Tumori 80:209-211
[Crossref] [Googlescholar] [Indexed]
- Aydin B, Aksu O, Asci H, Kayan M, Korkmaz H (2018) A rare cause of pituitary apoplexy: cabergoline therapy. Acta Endocrinol (Buchar) 14:113-116.
[Crossref] [Googlescholar][Indexed]
- Ranabir S, Baruah MP (2011) Pituitary apoplexy. Indian J Endocrinol Metab Suppl 3:S188-196.
- Briet C, Salenave S, Bonneville JF, Laws ER, Chanson P (2015) Pituitary Apoplexy. Endocr Rev 36:622-645.
- Guijt MC, Zamanipoor Najafabadi AH, Notting IC, Pereira AM, Verstegen MJ, et al. (2022) Towards a pituitary apoplexy classification based on clinical presentation and patient journey. Endocrine 76:132–141.
- Murad-Kejbou S, Eggenberger E (2009) Pituitary apoplexy: Evaluation, management and prognosis. Curr Opin Ophthalmol 20:456-61.
[Crossref] [Googlescholar] [Indexed]
- Ghadirian H, Shirani M, Ghazi-Mirsaeed S, Mohebi S, Alimohamadi M (2018) Pituitary apoplexy during treatment of prolactinoma with Cabergoline. Asian J Neurosurg 13:93-95.
- Oertel, Teping F (2022) Editorial “pituitary apoplexy-are visual deficits the only indication for emergent surgical intervention?”. Acta Neurochir 164:1125–1126.
[Crossref] [Googlescholar] [Indexed]
- Rajasekaran S, Vanderpump M, Baldeweg S, Drake W, Reddy N, et al. (2011) UK guidelines for the management of pituitary apoplexy. Clin Endocrinol (Oxf) 74:9-20.
[Crossref] [Googlescholar] [Indexed]
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi 


