About the Journal
International Journal of Ophthalmic Pathology is a peer-reviewed scholarly journal in the field of Ophthalmology that aims to publish the most complete and reliable source of information on the discoveries and current developments in the mode of research articles, review articles, case reports, short communications, etc. in all areas of Ophthalmology and making them accessible online freely without any restrictions or any other subscriptions to researchers worldwide.
International Journal of Ophthalmic Pathology focuses on the topics include, but are not restricted to: Ophthalmic studies of eye physiology, eye disorders along with the pathology studies on the neuro-ophthalmology, ophthalmic genetics, ocular surface physiology, ocular therapeutic pharmacology, ophthalmic oncology, pediatric ophthalmology and ocular pathology.
Review processing is performed by the editorial board members of International Journal of Ophthalmic Pathology or outside experts; at least two independent reviewers approval followed by editor approval is required for acceptance of any citable manuscript. Authors may submit manuscripts and track their progress through the system, hopefully to publication. Reviewers can download manuscripts and submit their opinions to the editor. Editors can manage the whole submission/review/revise/publish process.
Neuro Ophthalmology
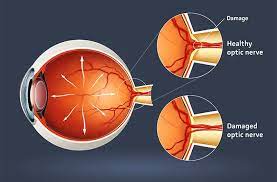
Neuro ophthalmology specially deals eye diseases with several neuro logical problems and several eye disorders. Neuro ophthalmology fall into two groups diseases affecting optic nerve and disease affecting eye movements.
Ophthalmic Surgery
Ophthalmic surgery also known as eye surgery are performed on the eye or its adnexa, typically by an ophthalmologist. There are different types of surgery performed by ophthalmologist.
Vision Rehabilitation
Vision rehabilitation is the process of treatment and education that helps individuals who are visually disabled attain maximum function, a sense of well being, a personally satisfying level of independence, and optimum quality of life. Function is maximized by evaluation, diagnosis and treatment including, but not limited to the prescription of optical, non-optical, electronic and/or other treatments. The rehabilitation process includes the development of an individual rehabilitation plan specifying clinical therapy and/or instruction in compensatory approaches.
Eye Diorders & Vision
Eye Disorders is the branch of the ophthalmic research which encompass on the study and reasearch on eye related disease which leads to the loss of vision.
Glaucoma
Glaucoma is group of ocular disorders which apparent grey–green color of the eye suffering from an attack of acute narrow-angle glaucoma. Several pathologists characterized that diseases result in due to raised of interocular pressure of the eye.
Optometry
Optimetry is a another type of health care profession which deals with eye and its related structures along with vision and visual system. Optometry person differs from the ophthalmic surgeon on the bases of their training and diagnose.
Ocular Immunology
Ocular immunology is branch of medicine which deals with diagnosis the eye and treating the patients with inflammatory eye diseases and also deals with immunology impacts several eye diseases and disorders.
Visual Impairment
Vision science is the scientific study of vision. Vision science encloses all studies of vision, such as how human and non-human organisms’ process visual information, how conscious visual perception works in humans, how to exploit visual perception for effective communication, and how artificial systems can do the same tasks. Vision science overlaps with or encompasses disciplines such as ophthalmology and optometry, neuroscience, psychology, optics and computer vision, etc.
Surgical Ophthalmology
It is branch of medicine deals with surgical procedure performed by the ophthalmologist. They are several surgical procedure deals by the ophthalmologist such as cataract surgery.
Cataract
Cataract is nothing but a clouding of the lens in the eye that leads to decrease in the vision. It may affect both eyes or one eye.
Refractive Surgery
It is a surgical remodeling the refractive state of eye to eliminate dependency of glasses or contact lens. They are different types of refractive sugery to improve the vision such as Lasik surgery.
External Eye Diseases
External Eye Diseases have several genetic disorders that lead to external eye disease. External eye disease is contagious and requires antibiotic treatment. Some of the list external eye disease are retinal disorders, tear disorders, cataract, refrarctive errors and corneal allergies.
Inflammatory Eye Diseases
The swelling in the ocular surface of the eye leads to disorders which have to treat immediately. Several inflammatory diseases occur due to the failure of autoimmune system in the eye. There are two types of inflammatory disease such as Uveitis and Scleritis.
Occuloplastics
Occuloplastics are specialist in the remodeling of the per orbital and facial tissues including the eyelids, eyebrows, forehead, cheeks, orbit and also deals with recontruction eye and its associated structure.
Ophthalmic Genetics
Ophthalmic genetics is a branch of medicine which deals with genetics behind the eye disorders and eye diseases, It is also includes the several technique in correcting the defective gene.
Diabetic Retinopathy
Diabetic retinopathy is the most common legal blindness disease which occurs between the ages of 20 to 65 years. Diabetic retinopathy is the most serious ocular complication which may affected in other ways.
Ophthalmic Research
Ophthalmic research is a branch of medicine pertaining to eye which deals with anatomy and diseases. Ophthalmic research focus on the eye search, eye infection, eye diseases and eye surgery.
Strabismus
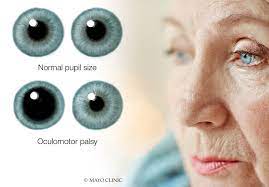
Its most common diseases due to misalignment of the eyes. It is due to failure three cranial nerves which are responsible for the eye movements.
Ophthalmic Pathology
Ophthalmic pathology which deals with diagnosis of the neoplastic and non-neoplastic diseases of the eye. This ophthalmic pathologist work closely with ophthalmic surgeon but they encompass with the pathology concepts.
Ocular Oncology
Ocular oncology is the branch of medicine deals with the various cancerous tumors of the eye. some of the most common tumors of the eye is retinoblastoma.
Impact Factor
2016 Journal Impact Factor is the ratio of the number of citations achieved in the year 2016 based on Google Search and Google Scholar Citations to the total number of articles published in the last two years i.e. in 2014 and 2015. Impact factor measures the quality of the Journal.
If ‘X’ is the total number of articles published in 2014 and 2015, and ‘Y’ is the number of times these articles were cited in indexed journals during 2016 then, impact factor = Y/X.
Fast Editorial Execution and Review Process (FEE-Review Process):
International Journal of Ophthalmic Pathology is participating in the Fast Editorial Execution and Review Process (FEE-Review Process) with an additional prepayment of $99 apart from the regular article processing fee. Fast Editorial Execution and Review Process is a special service for the article that enables it to get a faster response in the pre-review stage from the handling editor as well as a review from the reviewer. An author can get a faster response of pre-review maximum in 3 days since submission, and a review process by the reviewer maximum in 5 days, followed by revision/publication in 2 days. If the article gets notified for revision by the handling editor, then it will take another 5 days for external review by the previous reviewer or alternative reviewer.
Acceptance of manuscripts is driven entirely by handling editorial team considerations and independent peer-review, ensuring the highest standards are maintained no matter the route to regular peer-reviewed publication or a fast editorial review process. The handling editor and the article contributor are responsible for adhering to scientific standards. The article FEE-Review process of $99 will not be refunded even if the article is rejected or withdrawn for publication.
The corresponding author or institution/organization is responsible for making the manuscript FEE-Review Process payment. The additional FEE-Review Process payment covers the fast review processing and quick editorial decisions, and regular article publication covers the preparation in various formats for online publication, securing full-text inclusion in a number of permanent archives like HTML, XML, and PDF, and feeding to different indexing agencies.